Dental Advice from Doctor Humphrey
Cosmetic Dentistry, Sleep Apnea Devices & Emergency Dental Services in San Antonio TX
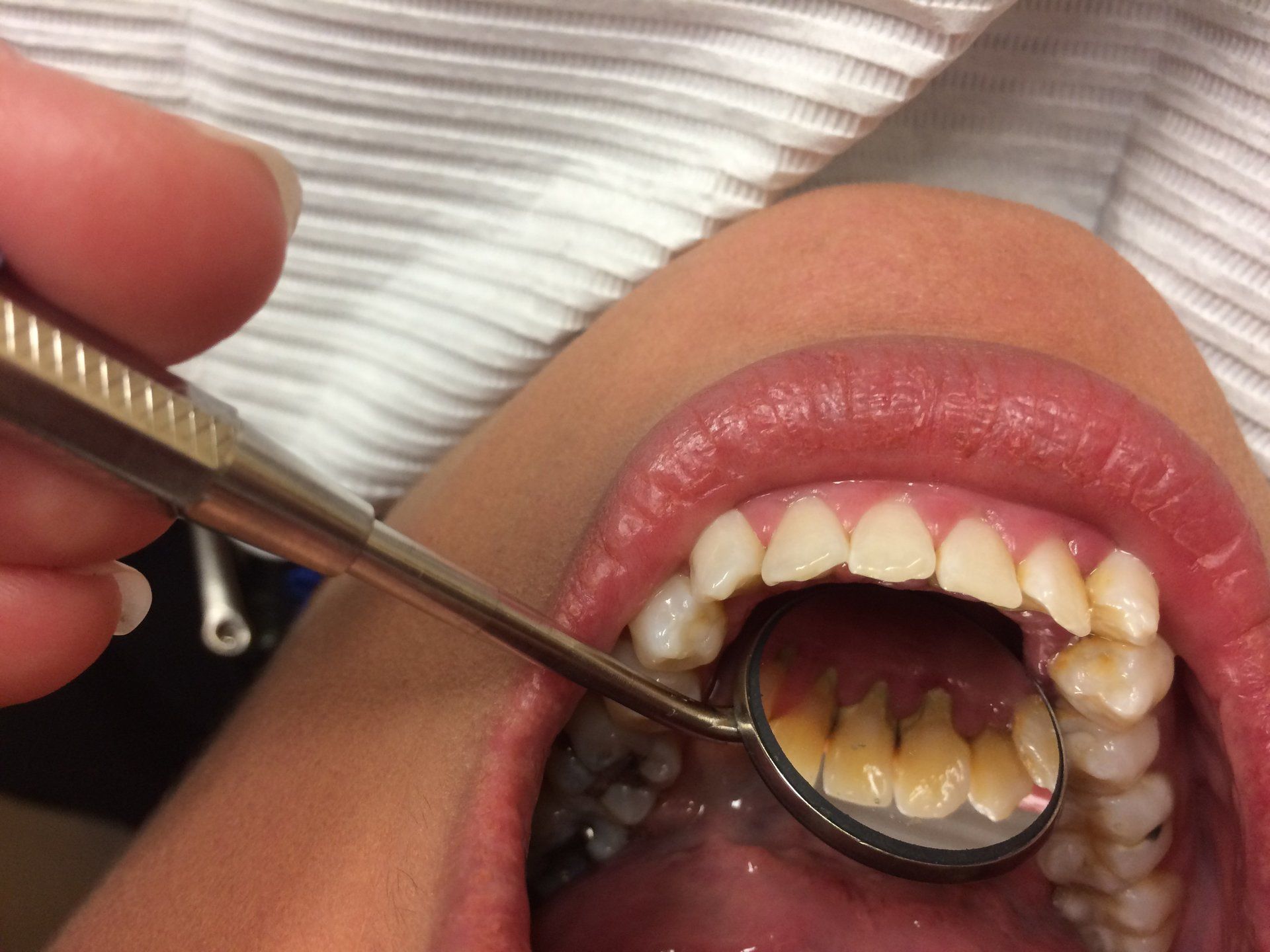
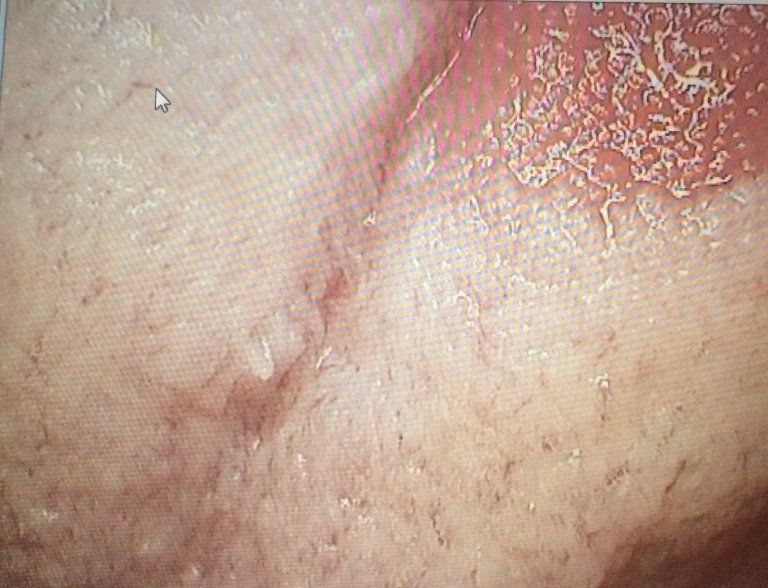
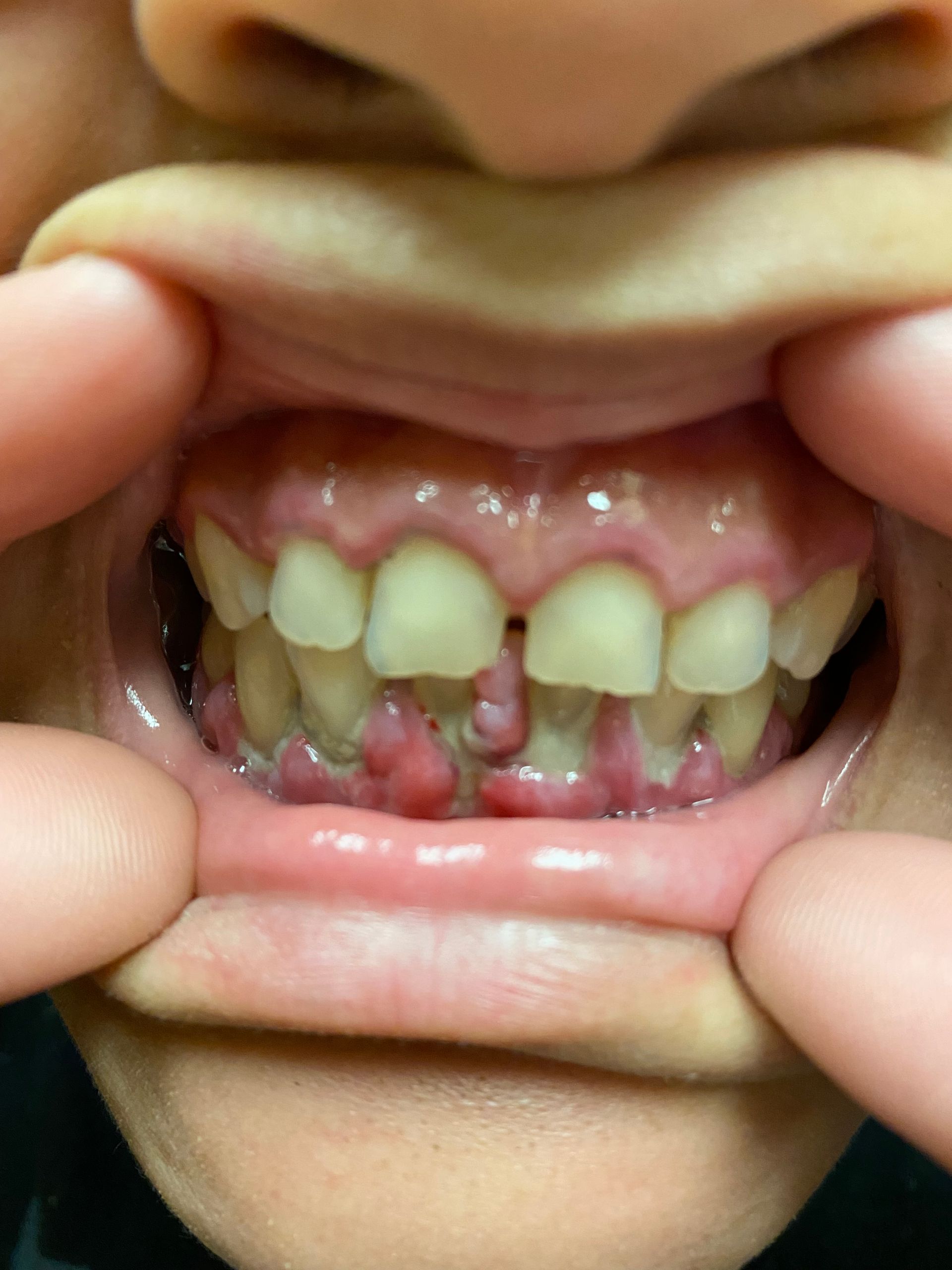
Dental Disease Process
In a nut shell, plaque is the dental adversary. It consists of various bacterial colonies forming every 24 hours whether or not food is ingested. It secretes an acidic waste product which burns the teeth and irritates the gums leading to caries and periodontal disease. Each day that plaque can sit on the teeth (including in between and under the gum line), it slowly hardens as it destroys tissue and deepens gum pockets making it more difficult to remove.
Prevention
Our office recommends the following oral hygiene program once daily:
- Pre-rinse or pre-brush with Plax (swish 1-5 minutes) Brush lightly for 10 seconds with each area of the brush, angling 45 degrees into the gum line with a circular vibrating motion; or use an electric brush.
- Floss in a figure eight movement rapidly stroking at least 6 times against both sides of the tooth. Bleeding may occur. The advanced technique includes a knot tied in the floss demonstrated at our office. Listerine is used next to reduce inflammation.
- Follow with a strong Fluoride applied to the gum line and rinsed after 30 minutes.
- Consider wearing a night guard to prevent wear and fractures.
For more helpful information visit the American Dental Association .
About Teeth
Teeth are not complicated to understand. The crown, or what is visible in the mouth, consists of an outer egg type shell. This outside layer, called enamel, is the hardest substance in the body; Harder than bone with great compressive strength, but weak in its tensile vigor. In other words, enamel can withstand the strong forces of your jaw muscles, but cannot flex if you bite sideways on a foreign object, or change from cold to hot quickly. Those conditions cause fractures to form which everyone has in their teeth, though some larger and more noticeable. Enamel is more resistance to acid from dental plaque and your stomach than other structures. Once a small hole is formed in the enamel, the disease can spread quickly through the dentin, decaying large areas of the tooth which can progress to the pulp leading to necrosis. Fluoride, if given to children topically and systemically early enough, combines with the enamel matrix strengthening its shield. In adults, extra fluoride may be applied topically if caries or exposed roots are problems. Dentin, the second layer of the crown structure and outer layer of the root, is much softer than enamel. Microscopically, it looks like a hard-natural sponge consisting of tubules. In dentin, the spaces are filled with moisture and nerve tentacles from the pulp. Any change in the water pressure, temperature, or chemistry send signals to the nerve resulting in pain. This structure is not resistance to acid or bacteria which can infect the pulp and cause the tooth to die.
The inner pulp structure of the crown or root is basically comprised of soft nerve and blood tissue housed in the hollow center of the tooth. The pulp which is necessary for tooth formation, later prevents the tooth from drying out and weakening. The nerve may repair itself after trauma, especially with young teeth. If the tooth tightens up, and no symptoms are present, have the tooth evaluated regularly for nerve health. Fractures can be better avoided by having a healthy pulp sensitive to foreign oral objects. If the nerve is removed, as in root canal therapy, the tooth dries out and cannot sense hard objects, leading to cracks. Root canal treated teeth may not last your lifetime. Therefore, it must be cover with a crown to prevent serious fractures.
Inflammation of the pulp is what causes the nerve to die. Excessive bruxism, malocclusion, deep caries, replacing large fillings or crowns, regularly drinking hot beverages, chewing on ice, trauma, deep fractures, periodontal disease, missing fillings, and rapid movement in orthodontics contribute to this common problem.
a.) Pulpitis: If you drink something very cold, and you feel a sharp, short pain, that is reversible pulpitis. The nerve is trying to repair itself, most commonly from recent dental treatment, a fracture, or trauma. Treat your tooth like a sprained ankle. Take Advil and stay off it. If the tooth doesn't start to feel better after a couple weeks or worsens and the pain to cold lingers, or the pain is felt even with room temperature water, see your dentist. You may have a fracture, or irreversible pulpitis; the tooth cannot heal itself and root canal treatment is required.
b.) Dentinal Sensitivity: Exposed roots at the gum line or between the teeth, can also be sensitive to cold or flossing from grinding, heavy brushing, tobacco, recent dental treatment. Try to locate the tooth. Is the pain from the root area or from the whole tooth? Do you see a black area or hole? If not, and the pain is only from the root, use a very strong pure topical fluoride gel, such as Gel Kam®, and toothpaste for sensitive teeth along the root and between the teeth with a small interproximal brush, until sensitivity goes away. Gel Kam® also comes unflavored, and should be used at room temperature
a.) Reversible Pulpitis- exposing a tooth to heat elicits a sharp, short, non lingering pain. The nerve is telling you that it is being irritated from a deep cavity, a fracture, recent dental treatment, or trauma.
b.) Irreversible Pulpitis/Pulp Necrosis- the delayed pain from hot now lingers or throbs for over a minute signaling that the soft tissue nerve has died and is forming an abscess. Both conditions are serious requiring immediate dental treatment.
a.) Slight pain from this is usually from an irritated or inflamed periodontal ligament that which holds the root to the bone. Common causes are from bruxism or grinding/clenching, sinus infection, orthodontics, trauma, or dental treatment. A simple cavity would not be the cause. It should go away with time especially if you can fabricate a temporary night guard to alleviate the stress. Take Advil, don't chew gum, and have a soft diet.b.) Severe pain to tapping, with other symptoms, may indicate an abscess. See your dentist.
a.) Biting down pain-The PDL is irritated. Common causes, involving more than one tooth, are grinding/clenching, sinus infection, or orthodontics. When only one tooth is sensitive, trauma, or fracture is most likely. In some cases, with more severe pain, an abscess may be present. A high spot on a filling or crown/cap can also mimic this symptom, but could be easily remedied with an adjustment by your dentist. A growth or tumor may push a tooth up, and abscess tends to burst out the side.
b.) Lifting off pain- almost always a fracture which causes more pain as the bite is released than when biting down on the object, requiring a crown to prevent further fracture movement. Usually the tooth will only hurt when biting on one edge or when chewing at a certain angle in cases of a fracture.